Evaluating the importance of chronic pain acceptance amid the opioid epidemic.
Author |

The opioid epidemic has left us scrambling for solutions that simultaneously address the need to manage chronic pain and solve the problems of opioid addiction and overdose that have plagued the nation. In the process of formulating a solution, many have reflected on what led us to this point. While some have rightly highlighted the role of marketing practices of opioid manufacturers as critical in the making of this epidemic, a number of broader cultural factors also bear responsibility.
In the late 1990s, there began a national push to evaluate pain as a fifth vital sign and treat it with commensurate seriousness. This effectively reinforced a pre-existing dominant American notion that pain is a problem that must be solved. In contrast, some cultural traditions hold that pain is natural and expected, and need not prevent one from living a meaningful life.
Interestingly, around the same time as the emergence of pain as a fifth vital sign, the concept of chronic pain acceptance began to gain traction in the field of pain psychology. Pain acceptance reflects the attitude that pain, while not preferable, is OK, and that even chronic pain does not inevitably prevent a person from getting on with what they value in life. The thinking here is that pain acceptance can provide a sort of pressure-release valve that relinquishes people from the often constant struggle to achieve pain relief. In the context of chronic pain, experiencing occasional breaks during which pain is sometimes allowed rather than resisted can create mental and emotional space. In this space, the person can think about what else they want from life, besides pain relief.
In the late 1990s, there began a national push to evaluate pain as a fifth vital sign and treat it with commensurate seriousness. This effectively reinforced a pre-existing dominant American notion that pain is a problem that must be solved.
Across many studies in various clinical populations, pain acceptance has been shown to be related to better outcomes, including lower emotional distress and better functional outcomes, for people with chronic pain. What prior research does not speak to is how pain acceptance relates to the use of other types of pain management strategies, such as medication use. I recently led a study that examined how pain acceptance is related to the use of both opioid and non-opioid pain medications. This study, published in The Clinical Journal of Pain, was conducted with people who have chronic pain secondary to spinal cord injury, a condition in which side effects from pain medications, even non-narcotic medications, can be quite dangerous.
We found that those with higher pain acceptance reported significantly lower use of all types of pain medications; every one-unit increase on the pain acceptance scale corresponded with 3% lower odds of opioid use. The association between pain medication usage and pain acceptance was significant, above and beyond the effects of the level of depressive symptoms, pain intensity, and pain distribution.
The data supported our idea that those who were more accepting of pain relied less on pain medications, and that this association was independent of the effects of mood, as well as the intensity and distribution of pain. These findings suggest that pain acceptance has a role to play in helping individuals reduce reliance on opioid medications and indicate a way forward for our collective attitude toward pain. Retaining the emphasis in medicine of evaluating pain as a "vital sign" need not be abandoned. Indeed, I would advocate for greater communication about pain in an effort to collaboratively develop more individualized and multi-modal pain treatment strategies.
We found that those with higher pain acceptance reported significantly lower use of all types of pain medications; every one-unit increase on the pain acceptance scale corresponded with 3% lower odds of opioid use.
It bears mentioning that people with chronic pain often feel upset when they hear pain professionals talk about acceptance of chronic pain. It's admittedly easy to hear "resignation" in the word acceptance, as if we are asking people to give up on the hope that we will find more pain relief than they have now. Patients may feel it's a way to relinquish our professional responsibility to help them manage their pain.
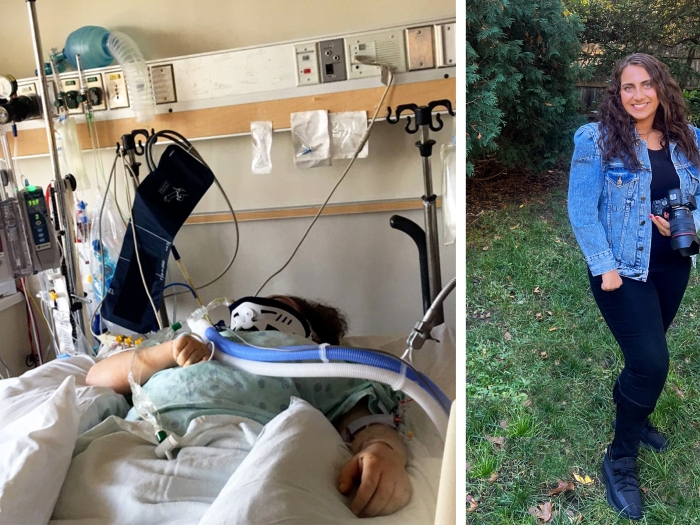
As someone who has lived with chronic pain for over a decade, I get it. But I also understand that my pain is not likely to ever go away completely, so accepting this reality is going to be necessary if I want to avoid a pain-focused life. Although the title of this article implies an either/or approach, pain acceptance will likely result in the greatest benefit for people with chronic pain when used in concert with other approaches, which may include medications.
People who are higher in pain acceptance may feel less of a need to relieve all pain, use a broader and more flexible repertoire of coping strategies, and rely less on pain medications as a result. Pain acceptance can be increased through psychological treatments, including cognitive behavioral therapy, acceptance and commitment therapy, and mindfulness-based stress reduction. Future studies that examine the effects of these behavioral treatments, and the role of pain acceptance in avoiding initiation of opioid medication and tapering from opioids, are warranted. The opioid epidemic is a complex puzzle, and this approach could be an important piece of the solution.
Anna Kratz, Ph.D., is an associate professor of physical medicine and rehabilitation. The study she references appears in the April 2018 issue of The Clinical Journal of Pain.